What is the most common cause of respiratory alkalosis?
.
Similarly, you may ask, what is respiratory alkalosis?
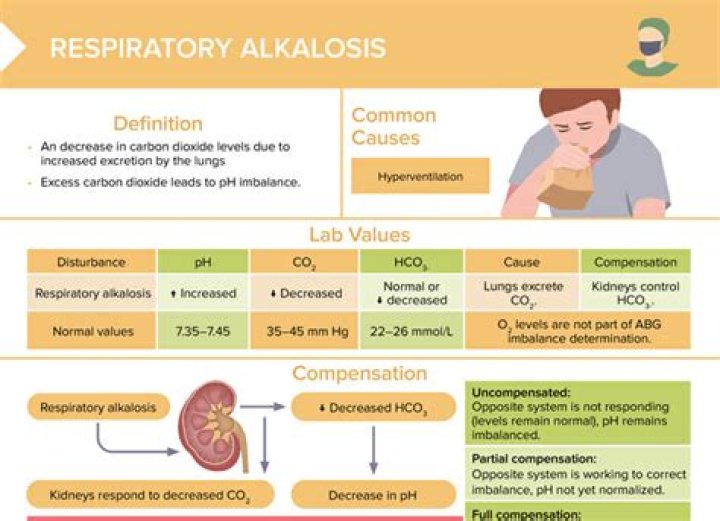
Respiratory alkalosis is a medical condition in which increased respiration elevates the blood pH beyond the normal range (7.35–7.45) with a concurrent reduction in arterial levels of carbon dioxide. This condition is one of the four basic categories of disruption of acid–base homeostasis.
Subsequently, question is, how common is respiratory alkalosis? In chronic respiratory alkalosis, the PaCO2 level is below the lower limit of normal, but the pH level is relatively normal or near normal due to compensatory mechanisms. Respiratory alkalosis is the most common acid-base abnormality observed in patients who are critically ill.
People also ask, how does the body fix respiratory alkalosis?
The condition will likely resolve if a person or doctor corrects the underlying cause. The body may try to self-correct the pH imbalance that comes with respiratory alkalosis, such as by having the kidneys increase excretion of alkaline and reduce excretion of acid.
What is alkalosis and what causes it?
Alkalosis is excessive blood alkalinity caused by an overabundance of bicarbonate in the blood or a loss of acid from the blood (metabolic alkalosis), or by a low level of carbon dioxide in the blood that results from rapid or deep breathing (respiratory alkalosis).
Related Question AnswersWhat drugs cause respiratory alkalosis?
Iatrogenic causes of respiratory alkalosis include medications like progesterone, methylxanthines (e.g., theophylline), salicylates (also cause primary metabolic acidosis), catecholamines and nicotine as well as excessive minute ventilation provided by mechanical ventilation (especially in chronic obstructive pulmonaryHow does alkalosis affect the body?
Alkalosis occurs when your body has too many bases. It can occur due to decreased blood levels of carbon dioxide, which is an acid. It can also occur due to increased blood levels of bicarbonate, which is a base. This condition may also be related to other underlying health issues such as low potassium, or hypokalemia.How do you detect respiratory alkalosis?
- Use pH to determine Acidosis or Alkalosis. ph. < 7.35. 7.35-7.45.
- Use PaCO2 to determine respiratory effect. PaCO2. < 35.
- Assume metabolic cause when respiratory is ruled out. You'll be right most of the time if you remember this simple table: High pH.
- Use HC03 to verify metabolic effect. Normal HCO3- is 22-26. Please note:
What is the treatment for alkalosis?
Metabolic Alkalosis Treatment & Management- Carbonic Anhydrase Inhibitors.
- Acids.
- Potassium-Sparing Diuretics.
- Angiotensin-Converting Enzyme Inhibitors.
- Potassium Supplements.
- Fluid Replacements.
- Corticosteroids.
- Nonsteroidal Anti-inflammatory Agents.
What are the symptoms of alkalosis?
Symptoms of alkalosis can include any of the following:- Confusion (can progress to stupor or coma)
- Hand tremor.
- Lightheadedness.
- Muscle twitching.
- Nausea, vomiting.
- Numbness or tingling in the face, hands, or feet.
- Prolonged muscle spasms (tetany)
What are the symptoms of acidosis and alkalosis?
Acute metabolic acidosis may also cause an increased rate and depth of breathing, confusion, and headaches, and it can lead to seizures, coma, and in some cases death. Symptoms of alkalosis are often due to associated potassium (K+) loss and may include irritability, weakness, and muscle cramping.What happens when pO2 is high?
It primarily measures the effectiveness of the lungs in pulling oxygen into the blood stream from the atmosphere. Elevated pO2 levels are associated with: Increased oxygen levels in the inhaled air. Polycythemia.What are signs and symptoms of respiratory acidosis?
Initial signs of acute respiratory acidosis include:- headache.
- anxiety.
- blurred vision.
- restlessness.
- confusion.
How does the body compensate for hypercapnia?
Hypercapnia in chronic respiratory acidosis can persist without dangerously acidic blood because of the body's responses to compensate. The kidneys get rid of more acid and reabsorb more base to try and create a balance.How does the body compensate for metabolic alkalosis?
Compensation for metabolic alkalosis occurs mainly in the lungs, which retain carbon dioxide (CO2) through slower breathing, or hypoventilation (respiratory compensation). CO2 is then consumed toward the formation of the carbonic acid intermediate, thus decreasing pH. Respiratory compensation, though, is incomplete.How do you fix respiratory acidosis?
Treatment is aimed at the underlying disease, and may include:- Bronchodilator medicines and corticosteroids to reverse some types of airway obstruction.
- Noninvasive positive-pressure ventilation (sometimes called CPAP or BiPAP) or a breathing machine, if needed.
- Oxygen if the blood oxygen level is low.


