What is a Category 1 pressure ulcer
Intact skin with non-blanchable redness of a localised area usually over a bony prominence. Darkly pigmented skin may not have visible blanching; its colour may differ from the surrounding area.
What is a Category 2 pressure ulcer?
A grade 2 pressure ulcer is defined as partial-thickness skin loss involving the epidermis, dermis or both. The ulcer is superficial and presents clinically as an abrasion or blister (Figure 2).
What are the categories of pressure ulcers?
- Category I – non-blanchable erythema.
- Category II – partial thickness skin loss.
- Category III – full thickness skin loss.
- Category IV – full thickness tissue loss.
- Deep tissue injury (DTI) – depth unknown.
What is a Stage 1 pressure injury?
Pressure injuries are described in four stages. Stage 1 sores are not open wounds. The skin may be painful, but it has no breaks or tears. The skin appears reddened and does not blanch (lose color briefly when you press your finger on it then remove your finger).What is a Category 3 ulcer?
Category III pressure ulcers are defined as being of full thickness skin loss, where the subcutaneous fat may be visible to the naked eye, but the skin damage has not exposed bone, tendon or muscle. Slough may be present but does not obscure the depth of tissue loss and may include undermining and tunneling.
What is a Category 4 pressure ulcer?
Category 4 pressure ulcer Full thickness tissue loss with exposed bone, tendon or muscle. Slough or eschar may be present on some parts of the wound bed. Often include undermining and tunneling. The depth of a Category 4 pressure ulcer varies by. anatomical location.
How would you describe Stage 1 pressure ulcer?
Stage 1 pressure injuries are characterized by superficial reddening of the skin (or red, blue or purple hues in darkly pigmented skin) that when pressed does not turn white (non-blanchable erythema). If the cause of the injury is not relieved, these will progress and form proper ulcers.
Are Stage 1 pressure ulcers Blanchable?
Stage 1: Intact skin with non- blanchable redness of a localized area usually over a bony prominence. Darkly pigmented skin may not have visible blanching; its color may differ from surrounding area.What do Stage 1 bedsores look like?
Stage 1 bedsores typically appear as red-colored patches of skin that do not blanch. This means that the red-colored patch of skin does not turn white when a finger is pressed upon the irritated area. On a dark-skinned patient, a stage 1 bedsore may simply appear to be a different color than the surrounding skin.
How long does it take for a Stage 1 pressure ulcer to develop?Findings from the three models indicate that pressure ulcers in subdermal tissues under bony prominences very likely occur between the first hour and 4 to 6 hours after sustained loading.
Article first time published onWhat are the 4 stages of pressure ulcers?
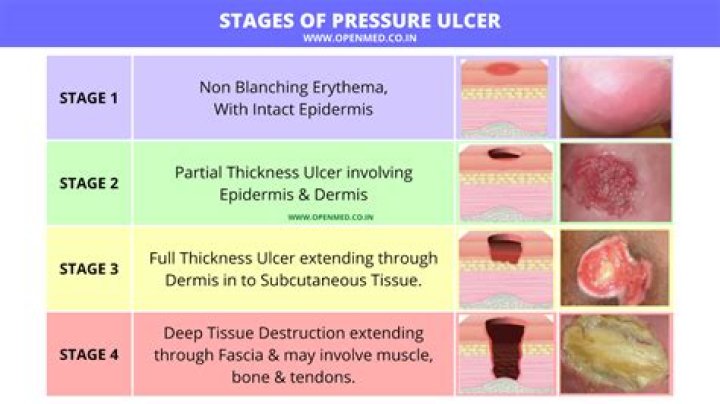
- Stage 1 Pressure Injury: Non-blanchable erythema of intact skin.
- Stage 2 Pressure Injury: Partial-thickness skin loss with exposed dermis.
- Stage 3 Pressure Injury: Full-thickness skin loss.
- Stage 4 Pressure Injury: Full-thickness skin and tissue loss.
What are the 5 stages of pressure ulcers?
- Stage 1. The area looks red and feels warm to the touch. …
- Stage 2. The area looks more damaged and may have an open sore, scrape, or blister. …
- Stage 3. The area has a crater-like appearance due to damage below the skin’s surface.
- Stage 4. The area is severely damaged and a large wound is present.
How are stage 4 pressure ulcers treated?
- Antibiotics. Giving patients bacteria-destroying medicine to treat infections.
- Debridement. Removing any damaged, infected, or dead tissue from the bedsore.
- Skin Grafts. Covering the affected area with healthy skin.
How do you Categorise a wound?
- Class 1 wounds are considered to be clean. They are uninfected, no inflammation is present, and are primarily closed. …
- Class 2 wounds are considered to be clean-contaminated. …
- Class 3 wounds are considered to be contaminated. …
- Class 4 wounds are considered to be dirty-infected.
What causes stage 3 pressure ulcer?
Bedsores form when blood flow to the skin is cut off, causing healthy tissue to die and an abrasion (open wound) to appear. The longer the bedsore is left untreated, the deeper the wound may become. Stage 3 bedsores occur when stage 2 bedsores fail to heal and the sore deepens into the patient’s skin.
What type of dressing is used on a Stage 1 pressure ulcer?
Semi-transparent hydrocolloid dressings may be used over reddened skin (Category/Stage I pressure ulcers) as it is possible to observe for deterioration without removing the dressing. The gel that forms during use of a hydrocolloid dressing makes removal easy and atraumatic.
How do you treat Epibole?
Treatment for epibole involves reinjuring the edges and opening up the closed tissue, which renews the healing process. Options include conservative or surgical sharp debridement, treatment with silver nitrate, and mechanical debridement by scrubbing the wound edges with monofilament fiber dressings or gauze.
What does Unstageable wound mean?
Unstageable. Definition. • Full thickness tissue loss in which actual. depth of the ulcer is completely obscured by slough (yellow, tan, gray, green, or brown) and/or eschar (tan, brown, or black) in the wound bed.
What is Stage 3 wound?
Depth of the Wound A stage 3 bedsores is a deep tissue injury. It is a tunneling wound that penetrates the top layers of skin and underlying tissue but not the bone or muscle. Seek immediate medical attention if your loved one has or may have a stage 3 bedsore.
How are Stage 3 pressure ulcers treated?
You must seek immediate medical treatment if you have a stage 3 pressure ulcer. These sores need special attention. Your doctor may prescribe antibiotic therapy and remove any dead tissue to promote healing and to prevent or treat the infection.
How would you describe Stage 3 pressure ulcer?
Stage 3 involves the full thickness of the skin and may extend into the subcutaneous tissue layer; granulation tissue and epibole (rolled wound edges) are often present. At this stage, there may be undermining and/or tunneling that makes the wound much larger than it may seem on the surface.
How do you get rid of stage 1 bedsores?
Stage 1 bedsores should also be washed with mild soap and water, then dried. Caretakers should continue to help patients move regularly and monitor their skin to make sure they don’t develop new sores. Other ways to treat bedsores include improving nutrition, increasing fluid intake and reducing friction when moving.
What is the fastest way to get rid of bed sores?
Baby powder will heal the sores faster. Baby powder makes the area dry and in turn prevents infection from spreading. It is important to keep the sores dry as it heals faster. Clean the affected areas with a disinfectant and then sprinkle baby powder to completely cover the wound.
What is the fastest way to heal a pressure ulcer?
If the affected skin isn’t broken, wash it with a gentle cleanser and pat dry. Clean open sores with water or a saltwater (saline) solution each time the dressing is changed. Putting on a bandage. A bandage speeds healing by keeping the wound moist.
Is a Blanchable wound good?
Tissue exhibiting blanchable erythema usually resumes its normal color within 24 hours and suffers no long-term damage. However, the longer it takes for tissue to recover from finger pressure, the higher the patient’s risk for developing pressure ulcers.
What does red and blanching mean?
Blanching redness = normal reaction Gently press the reddened area if it blanches white (as the blood is pushed out of the capillaries) then goes red again (as the capillaries refill) this is a normal reaction. This is Blanching Erythema (redness).
What is the difference between Slough and Eschar?
There are two main types of necrotic tissue present in wounds: eschar and slough. Eschar presents as dry, thick, leathery tissue that is often tan, brown or black. Slough is characterized as being yellow, tan, green or brown in color and may be moist, loose and stringy in appearance.
What are the early signs of pressure ulcers?
- Unusual changes in skin color or texture.
- Swelling.
- Pus-like draining.
- An area of skin that feels cooler or warmer to the touch than other areas.
- Tender areas.
Why don't you get bed sores when you sleep?
We normally move about constantly, even in our sleep. This stops pressure sores developing. People who are unable to move around tend to put pressure on the same areas of the body for a long time. If you are ill, bedridden or in a wheelchair, you are at risk of getting pressure sores.
Are bed sores painful?
Bedsores can be extremely painful. It is essentially an open wound, and usually develops in areas of the body that are hard to avoid putting pressure on. Even the most mundane of activities can cause serious pain when a patient has a bedsore. A bedsore is also known as a pressure sore or ulcer, or a decubitus ulcer.
What does it mean when a bed sore turns black?
Eschar refers to the dead tissue component of a bed sore or other wound, such as a burn injury. It appears as a patch of dead skin covering the bed sore. Eschar may be black, brown, or tan in appearance.