What happens in G6PD deficiency?
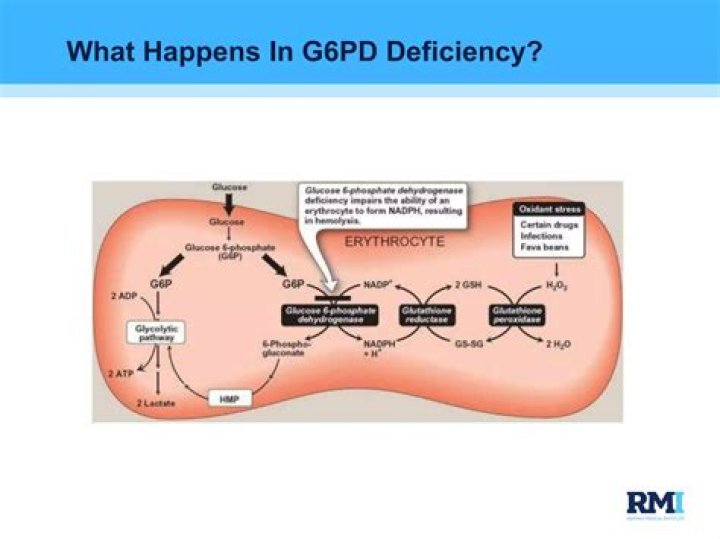
What happens in G6PD deficiency?
In people with G6PD deficiency, either the red blood cells do not make enough G6PD or what they do make doesn’t work as it should. Without enough G6PD to protect them, the red blood cells break apart. This is called hemolysis (hih-MOL-ih-sis).
What is the role of Phosphoglucomutase?
Phosphoglucomutase (EC 5.4. 2.2) is an enzyme that transfers a phosphate group on an α-D-glucose monomer from the 1 to the 6 position in the forward direction or the 6 to the 1 position in the reverse direction. More precisely, it facilitates the interconversion of glucose 1-phosphate and glucose 6-phosphate.
What happens when glucose-6-phosphate is absent during carbohydrate metabolism?
In GSDI, the absence of G6Pase activity leads to the accumulation of G6P in the liver and consequently the accumulation of glycogen and lipids, responsible for hepatomegaly and hepatic steatosis.
How does deficiency of G6PD produce hemolytic anemia?
It is when the body doesn’t have enough of an enzyme called G6PD (glucose-6-phosphate dehydrogenase). This enzyme helps red blood cells work correctly. A lack of this enzyme can cause hemolytic anemia. This is when the red blood cells break down faster than they are made.
What is the pathophysiology of G6PD deficiency?
Pathophysiology of G6PD Deficiency G6PD deficiency renders RBCs susceptible to oxidative stress, which shortens RBC survival. Hemolysis occurs following an oxidative challenge, commonly after fever, acute viral or bacterial infections, and diabetic ketoacidosis.
What cells are usually seen in patients with G6PD deficiency?
Glucose-6-phosphate dehydrogenase deficiency is a genetic disorder that affects red blood cells, which carry oxygen from the lungs to tissues throughout the body. In affected individuals, a defect in an enzyme called glucose-6-phosphate dehydrogenase causes red blood cells to break down prematurely.
Why does the defect in G6PD lead to oxidation of hemoglobin?
In G6PD deficiency, decreased NADPH levels results in oxidative injury of cell membranes, which may lead to hemolytic anemia. Hemoglobin is susceptible to oxidant damage, and denatured globin precipitates in the RBC forming Heinz bodies.
Is Phosphoglucomutase used in gluconeogenesis?
Glucose 1-phosphate is isomerized to G-6-P by phosphoglucomutase. G-6-P is dephosphorylated to glucose by glucose-6-phosphatase (G6Pase), which is present in the liver, but not muscle. G6Pase is a key regulatory enzyme in gluconeogenesis.
Why does a deficiency in glucose-6-phosphatase lead to hypoglycemia?
Glucose-6-phosphatase deficiency (glycogen storage disease type I) classically appears as severe hypoglycemia in neonates and infants and is caused by the inability to dephosphorylate glycogen subunits into glucose.
Why is it important that muscle cells lack glucose-6-phosphatase?
Liver cells express the transmembrane enzyme glucose 6-phosphatase in the endoplasmic reticulum. Muscle cells lack this enzyme, so myofibers use glucose 6-phosphate in their own metabolic pathways such as glycolysis. Importantly, this prevents myocytes from releasing glycogen stores they have obtained into the blood.