What are complications of percutaneous coronary intervention?
What are complications of percutaneous coronary intervention?
Complications can include:
- Injury to the heart arteries, including tears or rupture.
- Infection, bleeding, or bruising at the catheter site.
- Allergic reaction to the dye or contrast used.
- Kidney damage from the dye or contrast.
- Blood clots that can lead to stroke or heart attack.
Why is hypertension a risk factor for ACS?
Arterial hypertension is one of the main factors leading to atherogenesis and the development of vulnerable plaques whose instability or rupture (which in turn results in thrombosis and vessel occlusions) are responsible for the development of acute coronary syndromes (ACS).
Does Mi cause hypertension?
In general, the patient’s blood pressure is initially elevated (hypertension because of peripheral arterial vasoconstriction resulting from an adrenergic response to pain, anxiety, and ventricular dysfunction). However, it is not uncommon to have increased blood pressure as the precipitant of acute MI.
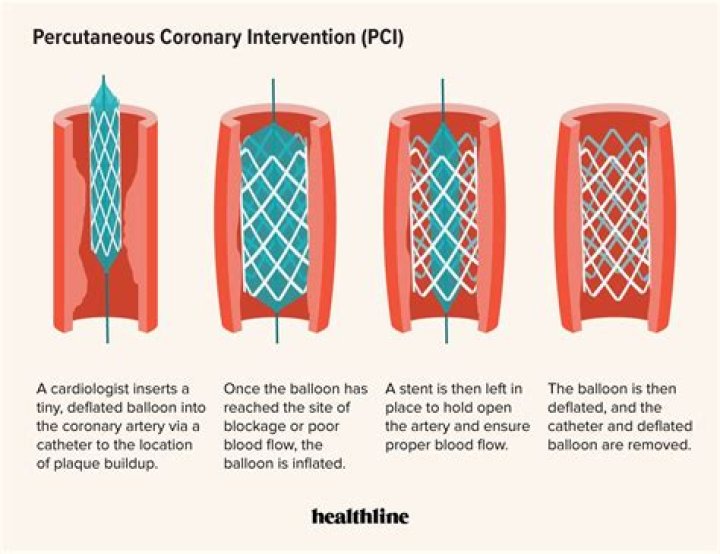
What happens during a primary percutaneous coronary intervention?
This is the basic PCI procedure. A catheter with a tiny, folded balloon on its tip is threaded through a blood vessel until it reaches the site where plaque buildup is causing a blockage. At that point, the balloon is inflated to compress the plaque against the walls of the artery.
What is the most serious complication of percutaneous transluminal coronary angioplasty?
The most serious complication of percutaneous coronary intervention results when there is an abrupt closure of the dilated coronary artery within the first few hours after the procedure.
What are the complications of angioplasty?
The risks associated with angioplasty and stents include:
- allergic reactions to medication or dye.
- breathing problems.
- bleeding.
- blood clots.
- infection.
- kidney damage.
- re-narrowing of your artery, or restenosis.
- rupture of your artery.
Which conditions are contraindications to therapy with β blockers in patients with ACS?
Contraindications for β-blockers administration are: hypotension (systolic blood pressure < 100 mmHg), bradycardia (heart rate < 50 bpm), phenomenon Raynaud, severe pneumonopathy (especially chronic obstructive and bronchial asthma), and severe renal insufficiency.
What happens to blood pressure during MI?
During a heart attack, the blood flow to a portion of your heart is blocked. Sometimes, this can lead to your blood pressure decreasing. In some people, there may be little change to your blood pressure at all. In other cases, there may be an increase in blood pressure.
Why does Mi cause hypotension?
Reduced left ventricular filling causes systemic hypotension, and less effective right-sided output results in jugular venous distention. The lung fields are clear (ie, there is no pulmonary edema) because the contractile dysfunction is proximal to the lungs.
What is the difference between angioplasty and PCI?
The stent is left in place permanently to allow blood to flow more freely. Coronary angioplasty is sometimes known as percutaneous transluminal coronary angioplasty (PTCA). The combination of coronary angioplasty with stenting is usually referred to as percutaneous coronary intervention (PCI).
What makes a PCI high risk?
High-risk PCI was defined as patients meeting one or more of the contemporary criteria described by the Interventional Council of ACC2: unprotected left main coronary artery disease, last remaining patent vessel, LVEF <35%, complex 3-vessel CAD, and comorbidities including severe aortic stenosis or severe mitral …