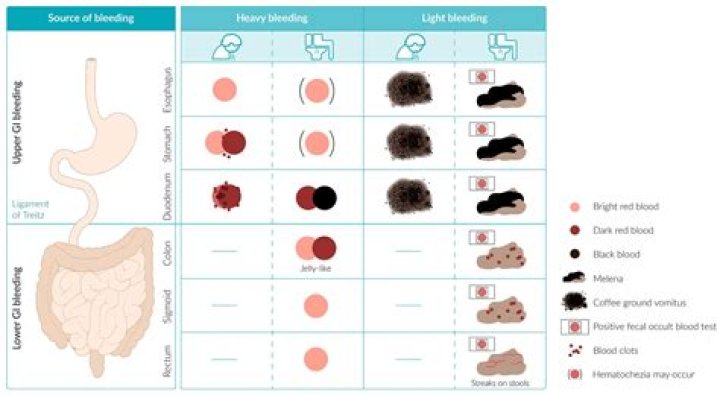
How is GI bleed diagnosed
Doctors most often use upper GI endoscopy and colonoscopy to test for acute GI bleeding in the upper and lower GI tracts. Upper GI endoscopy. In an upper GI endoscopy, your doctor feeds an endoscope down your esophagus and into your stomach and duodenum.
How do you test for a GI bleed?
The test used most often to look for the cause of GI bleeding is called endoscopy. It uses a flexible instrument inserted through the mouth or rectum to view the inside of the GI tract. A type of endoscopy called colonoscopy looks at the large intestine.
What is the most definitive indicator of a GI bleed?
Blood exiting the GI tract is the best and most definitive indicator of GI bleeding. It comes in three forms: hematemesis, hematochezia and melena. Hematemesis is bloody vomit, which can come as either frank red blood or “coffee-ground” colored. A patient with hematemesis is bleeding above the ligament of Treitz.
Can a blood test show GI bleeding?
The amount of GI bleeding may be so small that it can only be detected on a lab test, such as the fecal occult blood test. Other signs of GI bleeding include: Dark, tarry stools. Larger amounts of blood passed from the rectum.What does poop look like with a GI bleed?
Melena: Melena is a black, tarry stool that is caused by GI bleeding. The black color is due to the oxidation of blood hemoglobin during the bleeding in the ileum and colon. Melena also refers to stools or vomit stained black by blood pigment or dark blood products and may indicate upper GI bleeding.
How can the doctor tell if you have internal bleeding?
Your doctor may use lab tests and imaging tools to both identify the cause of your internal bleeding and measure the severity. For injuries, an imaging test may be all that’s necessary. An X-ray shows an image of your bones. A CT scan is an advanced X-ray that can see bones, tissues, and blood vessels.
Can a CT scan detect GI bleeding?
CT angiography is an accurate examination for identifying the source of acute GI bleeding. A meta-analysis of data from 672 patients with moderate to severe UGIB and/or LGIB revealed an overall sensitivity of 85% and a specificity of 92% for detection of the bleeding site.
Can ultrasound detect GI bleeding?
Overall, ultrasound is a rapid, noninvasive test that can be used to detect bowel-wall abnormalities in patients with lower GI bleeding while they are being prepared for colonoscopy, but it does not eliminate the need for rapid colonoscopic diagnosis and therapy.Is a GI bleed an emergency?
Acute GI bleeding can quickly become serious. If a person suddenly develops symptoms of a GI bleed, they should seek immediate medical help. Acute GI bleeds can also lead to shock, which is a medical emergency.
How can you tell the difference between upper and lower GI bleed?Upper GI bleeding includes hemorrhage originating from the esophagus to the ligament of Treitz, at the duodenojejunal flexure[13]. Lower GI bleeding is defined as bleeding that originates from a site distal to the ligament of Treitz[14].
Article first time published onIs bright red blood upper or lower GI bleed?
Upper GI bleeding occurs when irritation and ulcers of the lining of the esophagus, stomach, or duodenum result in bleeding. When this occurs, the child will vomit bright red blood, or dark looking flecks or clots that look like “coffee grounds”.
Can you survive a GI bleed?
Background. Some patients who have a gastrointestinal bleed or perforation will die. Risk of mortality is probably higher in older people, in people with concomitant diseases, or with large ulcers in the posterior duodenal bulb or on the lesser curvature..
Can a GI bleed heal itself?
Often, GI bleeding stops on its own. If it doesn’t, treatment depends on where the bleed is from. In many cases, medication or a procedure to control the bleeding can be given during some tests.
What color is lower GI bleed?
Acute colonic bleeding (or lower GI bleeding)—defined as that occurring from the colon, rectum, or anus, and presenting as either hematochezia (bright red blood, clots or burgundy stools) or melena—has an annual incidence of hospitalization of approximately 36/100,000 population, about half of that for upper GI …
How long does it take to recover from GI bleed?
Even in the presence of a low Hb level at discharge, an acceptable outcome is expected after endoscopic hemostasis for nonvariceal upper gastrointestinal bleeding. Recovery of the Hb level after discharge is complete within 45 days.
Can MRI detect bleeding in Colon?
CONCLUSION In conjunction with an intravascular contrast agent, 3D MRI permits accurate detection and localisation of gastrointestinal bleeding. The extent and evolution of intestinal bleeding can be determined with repeated data acquisition.
Do you feel pain when you have internal bleeding?
The symptoms of internal bleeding can vary from one case to the next. It can be sudden and rapid with extreme pain, shock, and fainting. Or, it can be slow and “silent” with few symptoms until the total loss of blood is extreme.
What happens if a GI bleed goes untreated?
Left untreated, severe gastrointestinal bleeding can result in a life-threatening loss of blood. Seek immediate medical care (call 911) for serious symptoms, pale skin or pallor and difficulty breathing, severe abdominal pain, vomiting blood or black material, or change in level of consciousness.
How do you fix a GI bleed?
- inject medicines into the bleeding site.
- treat the bleeding site and surrounding tissue with a heat probe, an electric current, or a laser.
- close affected blood vessels with a band or clip.
What does a GI bleed smell like?
Bright red blood from the anus. Bleeding can be streaks of blood or larger clots. It can be mixed in with the stool or form a coating outside the stool. If the bleeding starts further up in the lower GI tract, your child may have black sticky stool called “melena”, which can sometimes look like tar and smell foul.
What can you diagnose from abdominal ultrasound?
- Bladder stones.
- Enlarged spleen.
- Gallstones.
- Cholecystitis (gallbladder inflammation).
- Pancreatitis (inflamed pancreas).
- Cancer, such as stomach cancer or pancreatic cancer.
- Fatty liver disease.
- Abdominal aortic aneurysm (a bulge in the aorta wall in your midsection).
What does upper GI bleed poop look like?
Your stool might become darker and sticky, like tar, if bleeding comes from the stomach or upper GI tract. You may pass blood from your rectum during bowel movements, which could cause you to see some blood in your toilet or on your toilet tissue. This blood is usually bright red in color.
How do PPIs treat GI bleed?
PPIs reduce gastric acid secretion for up to 36 hours,41 thereby promoting healing of ulcers and erosions as well as stabilizing thrombi and decreasing rates of GI bleeding in patients on DAPT.
What are the risk factors for GI bleed?
- Chronic vomiting.
- Alcoholism.
- Medications, including but not limited to. Non-steroidal anti-inflammatories (NSAIDs); commonly used NSAIDs include. Aspirin. Ibuprofen (Advil) Naproxen (Aleve) Anticoagulants.
- Gastrointestinal surgery.
How serious is a lower GI bleed?
Lower GI bleeds are often less serious than upper GI bleeds, with only 4% of people hospitalized with the condition dying. Often, these deaths are related to other conditions rather than the bleed itself.
What color is your poop when you have an ulcer?
Black Tarry, Sticky Stools Bleeding in the stomach (from gastritis or an ulcer) or the intestines can change the color of the stool. If bleeding occurs in the stomach or the upper part of the small intestine, the stool may turn black and sticky, and be described medically as black, tarry stool (melena).
What color is your poop if you have internal bleeding?
Black or tarry stools with a foul smell are a sign of a problem in the upper digestive tract. It most often indicates that there is bleeding in the stomach, small intestine, or right side of the colon. The term melena is used to describe this finding.