Do you clamp a chest tube for transport
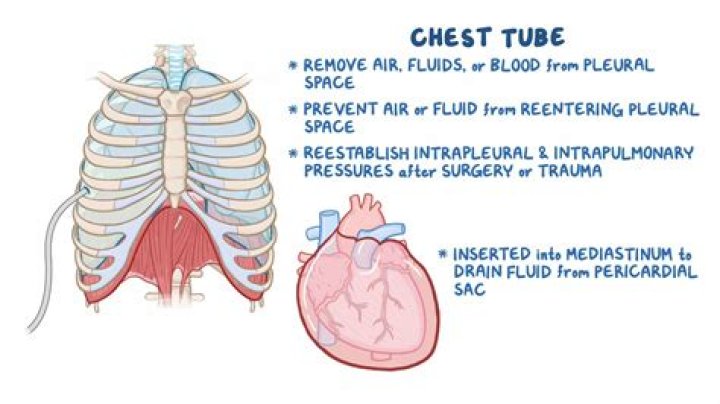
You should never clamp a chest tube during patient transport unless the chest drainage system becomes disrupted during patient movement, and then only if there is no air leak (7,9-11).
How do you transport a patient with a chest tube?
- Never lift drain above chest level.
- The unit and all tubing should be below patient’s chest level to facilitate drainage.
- Tubing should have no kinks or obstructions that may inhibit drainage.
- Ensure all connections between chest tubes and drainage unit are tight and secure.
Should a chest drain be clamped?
Clamping should be avoided if at all possible – clamping can cause a tension pneumothorax which leads to compression of the heart and a mediastinal shift which can be fatal. Don’t pass the chest drain over the patient – loss of gravity could cause contents to spill back into the pleural space.
How would you transport a patient with a chest tube to suction?
Mark the depth of the tube using a felt-tip marker and continually monitor during transport. If a drainage unit is used, be sure to keep it below the level of the chest. (Always use an appropriate chest drain system. Chest tubes should never be attached directly to wall or portable suction.Do you clamp chest tube before removal?
Chest tube clamping is recommended prior to removal if the patient receiving artificial respiration and has a history of severe air leak [19]. Clamping is not imposing radiation to the patients and is recommended to clamp six hours before removing the chest tube.
Should there be bubbling in the suction control chamber?
Bubbling in the Suction Control Chamber is Normal Nowadays, the suction pressure is controlled by the water level in the suction control chamber (in “wet” suction models). … If the suction pressure is set too high the water evaporates quicker from the drainage system and the nursing staff will have to refill it.
How do you insert a chest tube?
Incision: Using a scalpel, your doctor will make a small (¼- to 1 ½-inch) incision between your ribs, near the upper part of your chest. Where they make the incision depends on the reason for the chest tube. Insertion: Your doctor will then gently open a space into your chest cavity and guide the tube into your chest.
What is the difference between wet and dry suction chest tube?
Systems which employ a mechanical check-valve and a mechanical regulator are known as dry systems, whereas systems that retain a UWS but use a mechanical regulator are called wet-dry systems. Systems which use a water seal and water column regulator are called wet systems.How do you monitor chest tube drainage?
- Presence of air leaks.
- Fluctuation of water in water-seal chamber.
- Amount of suction.
- Amount of drainage and type.
- Presence of crepitus (subcutaneous emphysema)
- Breath sounds.
- Patient comfort level or pain level.
The few times you should clamp a chest tube are when: (I) you are performing a physician-ordered procedure such as sclerosing; (II) assessing for a leak or; (III) prior to removing the chest tube to determine if the patient can do without the chest tube (with a physician order).
Article first time published onHow much should a chest tube drain per hour?
7.1 Place container upright on floor. 7.2 Mark and date drainage, at eye level, on collection chamber. 7.3 Record. Pediatric: 3 mL/Kg/hour in a 3 hour period or 5 to 10 mL/Kg in any 1 hour period.
How do you manage a chest tube?
Management of Chest Tube The three options of how to manage a chest tube are suction, water seal, and clamping. When a new air leak is noted, the chest tube, connecting tubing, pleura-evac, and a patient’s wound should be examined for any loose connections or dislodgement of the tube.
What should patient do during chest tube removal?
Instruct the patient to practice taking deep breaths and holding them. To prevent air from re-entering the pleural space during tube removal, instruct the patient to hold the breath or to hum as you remove the tube. 5. After you’ve removed the dressing and sutures, clamp the tube.
How long does a chest tube stay in for a collapsed lung?
With a pneumothorax, healthcare providers will look at an X-ray to make sure all of the air has been removed, and the lung has expanded completely. Following lung cancer surgery, the tube will be left in place until only minimal drainage remains, often a period of three to four days.
How do I install an ICD drain?
- Secure the chest tube in place with a large silk suture (number 1 or 0) Go around the chest tube several times. Cinch down to create a small waist on the chest tube. Tie many knots. …
- A second suture should be used to close the incision, if there is additional space to avoid drainage or introduction of air.
Why don't you clamp a chest tube?
If you see visible clots, squeeze hand-over-hand along the tubing and release the tubing between squeezes to help move the clots into the CDU [1]. As a rule, avoid clamping a chest tube. Clamping prevents the escape of air or fluid, increasing the risk of tension pneumothorax.
How does chest tube suction work?
Closed chest drainage systems use gravity and/or suction to restore negative pressure and remove air, fluid, and/or blood from the pleural space so that the collapsed lung can re-expand.
What is Wall suction?
It consists of suction regulator and suction container. With connecting to vacuum outlet of hospital and as regulating pressure properly, it’s device to remove a foreign substance from patient.
Can a nurse insert a chest tube?
Advanced practice registered nurses and physician assistants perform chest tube insertions as well as trauma surgeons do.
What supplies do you need for chest tube insertion?
- Two guarded clamps.
- Sterile water.
- Vaseline gauze (Jelonet)
- 4 x 4 sterile dressing.
- Waterproof tape.
How do you confirm placement of a chest tube?
A finger is used to palpate the tract and feel for adhesions before insertion of the chest tube. Measure the length between the skin incision and the apex of the lung to estimate how far the chest tube should be inserted. If desired, place a clamp over the tube to mark the estimated length.
What should chest tube suction be set at?
The chest tube should initially be set to continuous suction at -20 mmHg to evacuate the air. Once the air leak has stopped, the chest tube should be placed on water seal to confirm resolution of the pneumothorax (water seal mimics normal physiology).
Should a chest tube have fluctuation?
You should see fluctuation (tidaling) of the fluid level in the water-seal chamber; if you don’t, the system may not be patent or working properly, or the patient’s lung may have reexpanded. Look for constant or intermittent bubbling in the water-seal chamber, which indicates leaks in the drainage system.
How do you set the level of suction in a dry suction chest drain?
Changing suction pressures Changing suction pressure is accomplished by adju- sting the rotary dry suction control dial located on the side of the drain. Dial down to lower the suction pres– sure and dial up to increase the suction pressure.
How much water should be in the water seal chamber?
LEVEL OF WATER IN WATER SEAL CHAMBER The water level should be at 2 cm. Water may need to be added due to evaporation. Add as needed through short suction tube. Water may need to be withdrawn if chamber is overfilled.
What is a one way valve chest tube?
The Heimlich valve is a one-way valve that prevents fluid and air from going back into your chest. The chest tube drains air and fluid from around the lung. The Heimlich valve allows the fluid and air to come out of your body into a drainage bag.
What does it mean to clamp a chest tube?
The practice of clamping the chest drain before removal in spontaneous pneumothorax appear safe. Clamping saved chest drain reinsertion in 11.8% of cases, and has the potential to save more if clamped for up to 24 h. However, clamping may result in more early recurrences.
Where do you insert chest drain?
A chest drain is a tube inserted through the chest wall between the ribs and into the pleural cavity to allow drainage of air (pneumothorax), blood (haemothorax), fluid (pleural effusion) or pus (empyema) out of the chest.
Where do you needle decompress?
Needle thoracocentesis is a life saving procedure, which involves placing a wide-bore cannula into the second intercostal space midclavicular line (2ICS MCL), just above the third rib, in order to decompress a tension pneumothorax, as per Advanced Trauma Life Support (ATLS) guidelines.
Can a nurse remove a chest tube?
A RN can safely remove mediastinal and/or pleural chest tubes with satisfactory training, supervised clinical practice and appropriate resources available for complication management.